Trusted Protection & Care
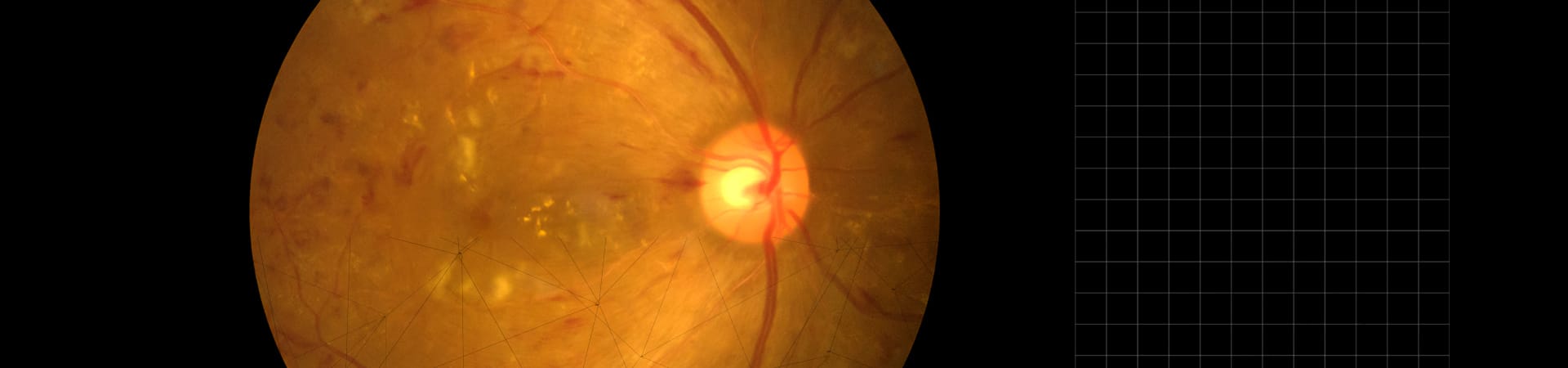
Staying aware of any changes to your eye health and vision can help you see clearly, longer. Most common eye diseases are asymptomatic in the early stages, which means attending regular comprehensive eye exams are imperative in safeguarding your vision.
Beyond eye exams, taking care of your overall health and well-being can keep your eyes healthy and protect your vision. Some useful tips for implementing into your daily routine are:
- Eat healthily. A diet rich in lutein and zeaxanthin can help prevent early development of cataracts and other eye diseases.
- Quit smoking. The chemicals in cigarettes and nicotine products can increase your risk of developing cataracts or macular degeneration.
- Wear sunglasses. UV rays can cause irreparable damage to your eyes and boost your chance of developing cataracts.
- Use safety glasses. If you work at a job where you use hazardous or airborne materials or play contact sports, protect your eyes from damage.
- Examine your Digital Eye Health®. Prevent digital eye strain and other causes of discomfort by practicing good usage habits while using digital devices.